Digital twins

Decentralized patients recruitment

Real-World Data

Passive Monitoring

Automated patient engagement
We've treated thousands of patients; built cutting edge digital health
platforms, and done billions of dollars in financial transactions in healthcare
We bet big on game changing teams and technologies in healthcare
Invest across digital health platforms
Early to mid-stage companies
Value-add with healthcare industry expertise
B2B, B2C, B2B2C, B2C2B models
Founder-centric partnership model
Significant follow-on capital
Invest across digital health platforms
B2B, B2C, B2B2C, B2C2B models
Value-add with healthcare industry expertise
Early to mid-stage companies
Founder-centric partnership model
Significant follow-on capital
Create funding plan that allows pursuit of aggressive growth plans
Facilitate introductions to a vast network of healthcare stakeholders
Share key lessons from past digital health product adoptions
Work with management team to optimize business model
Leadership
We have experienced the challenges of healthcare technology adoption. This makes us the ideal investors for innovative digital health entrepreneurs
Al in Healthcare Blog
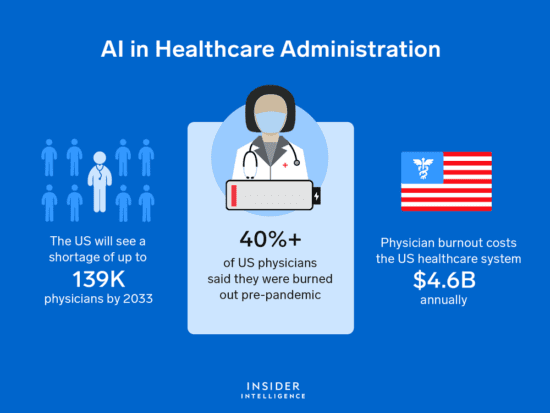
It’s estimated that about 25% of this $4 trillion is due to administration, which means that we spend...
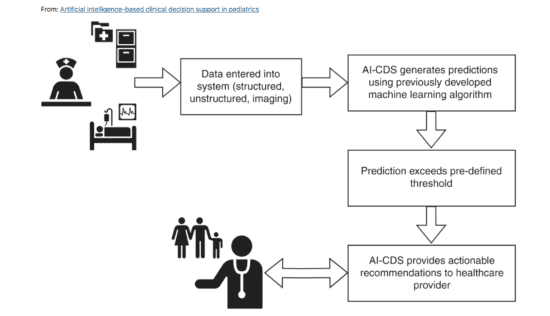
In a conversation with Kang Zhang, MD, one of the pioneers in the applications of healthcare AI, he...

As with clinical trials, regulatory submissions, pharmacovigilance, communicating with providers and patients, and monitoring social media for adverse...
Media

Poverty Impacting Women’s Healthcare Access: Gender Biased Artificial Intelligence and Infrastructure Creating Barriers
Poverty Impacting Women's Healthcare Access: Gender Biased Artificial Intelligence and Infrastructure Creating Barriers Mar 20, 2024, at 12.30...
Health AI: Hype vs Reality
A discussion of fact vs fiction in the applications of Artificial Intelligence in healthcare at the annual Wall...

Emerging Innovations in Healthcare #2: Mental Health (HYBRID)
Emerging Innovations in Healthcare (EIH) is a hybrid conference series by Mount Sinai Innovation Partners (MSIP), the commercialization arm of the Mount...